When I was making my rank list for residency, we ended up having to choose between a hospital in Baltimore that would let us stay at New Song and a hospital where I could get more obstetrical and surgical experience. We ended up staying in Baltimore to finish my training and I know we made the right choice, but that meant I had a steeper learning curve once we got to Bet Eman.
I spent a lot of time in Maryland learning how to deal with polysubstance abuse, getting patients off multiple unnecessary medications, and managing complex medical and mental health conditions in the primary care setting. Here, there just aren’t very many drugs to abuse, most people have a hard time getting necessary medications, and there’s almost no such thing as primary care. (I’ll write a blog post later about what’s similar between South Sudan and Baltimore, but today we’ll only talk about the salient differences!)
To be useful in our hospital setting in the long-term, I knew I would have to get a crash course in more advanced obstetrics. I got to assist on a handful of c-sections in my training, but I never held the knife myself– until this month!

As you probably know, South Sudan is one of the most dangerous places in the world to be a pregnant woman or an unborn child. For whatever reason, there’s a certain percentage of babies that, for their sake and/or their mothers’ sake, need to get cut out. My own daughter was born by c-section. Without access to a c-section, that 10-20% of pregnancies will end in death or severe disability for mom, baby, or both. This story from MSF reminds me of a lot of the patients we see on a daily basis.
While we are passionate about preventive medicine and community health to keep people from getting sick or needing to come to the hospital in the first place (and Bet Eman sees hundreds of prenatal patients a month to keep pregnant mothers healthy!), there are sometimes when you need an operation to stay alive. Hence, I’m learning how to do c-sections so we can provide this service to the community– and once I’m fully trained, I can teach others who will work in places in South Sudan I can’t take my family.

We’ve had a lot of short-term visitors the past few months that have helped to lighten the load at the hospital, so I’ve also gotten to learn from a bunch of different family doctors as well as our South Sudanese medical officer (she trained in Uganda and has been a tremendous mentor in navigating the tough medical and cultural issues I’ve encountered so far!) Everyone does things a little differently, which is great for my education as I learn a variety of techniques and rationales for various decisions.
I regret to inform my mother that all of that hype about playing a lot of video games improving one’s hand-eye coordination and making one a better surgeon is probably not true (although I haven’t tried my hand at laparoscopic surgery yet, so who knows? I still play computer games for fun and relaxation, though, just like I’m sure Jim Elliott did.) Both Dr. Jeff and I have vision issues, so we have to work a little more slowly and drive our nurse-anesthestist crazy by asking them to raise and lower the bed constantly.
I still love the primary care aspects of my job. I miss my patients in Baltimore and their multiple unnecessary medications. However, I also love doing surgeries (as long as they’re short!) and there is a serious need for good surgical care here in South Sudan. (If you’re interested in learning more about how surgeons are starting formal training programs to train the health workers Africa needs, check out the great work of the Pan-African Academy of Christian Surgeons.) I’m thankful that I got the opportunities I had to learn in Baltimore and that I have mentors here at Bet Eman who are teaching me some hardcore obstetrics after I’ve finished residency.
I’ve gotten to hold the scalpel about ten times in the past 3 weeks and I know that I still have a few dozen more to go before I’ll be anywhere near “independent.” Some of the cases had some pretty hairy complications and the physician I was operating with had to take over for a few minutes. But even on my first one, after I got the baby out one of our South Sudanese clinical officers took over to do the sewing. He’ll be cutting himself soon.
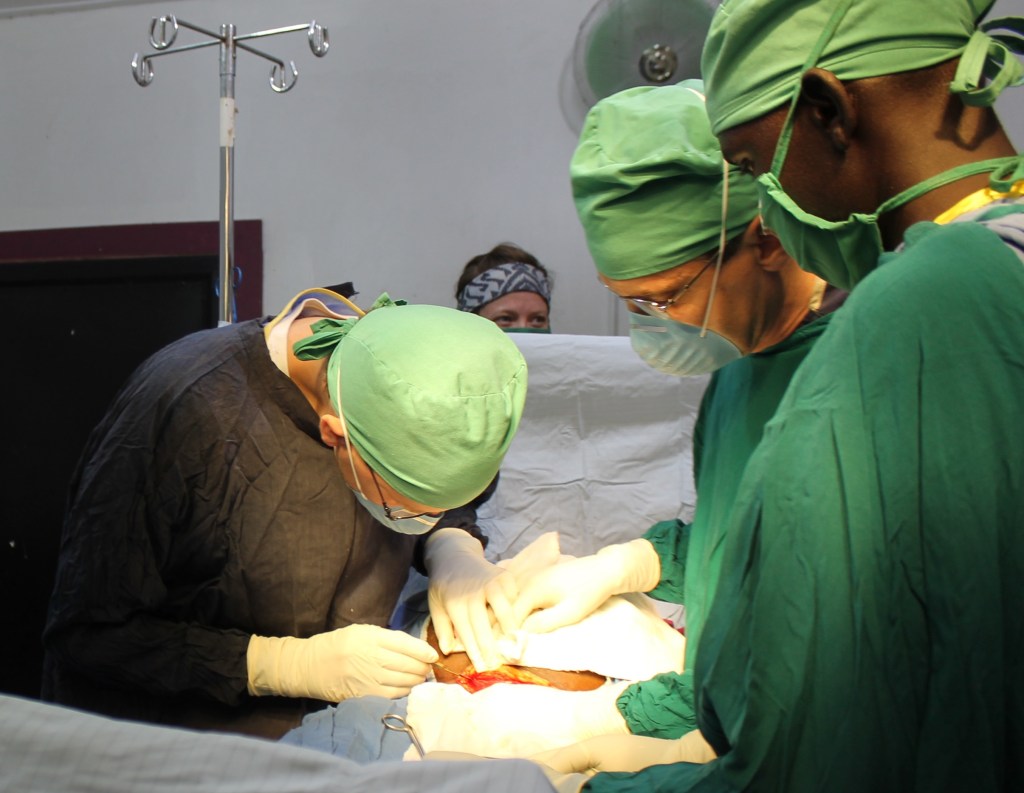
[somewhat bloody but tasteful picture of me delivering the baby’s head after the obligatory Weird Al video]




Leave a comment